PRIMARY CARE
Advanced Clinical Practice (ACP)
Advanced clinical practitioners (ACP) come from a range of professional backgrounds such as nursing, pharmacy, paramedics’ physiotherapy, and occupational therapy. They are healthcare professionals educated to Master’s Level and have developed the skills and knowledge to allow them to take on expanded roles and scope of practice caring for patients.
For all ACP queries please contact [email protected]
If you have not already, sign up to HEE’s ACP database, to get updates on different pieces of work that the Faculty is delivering.
Becoming an Advanced Practitioner
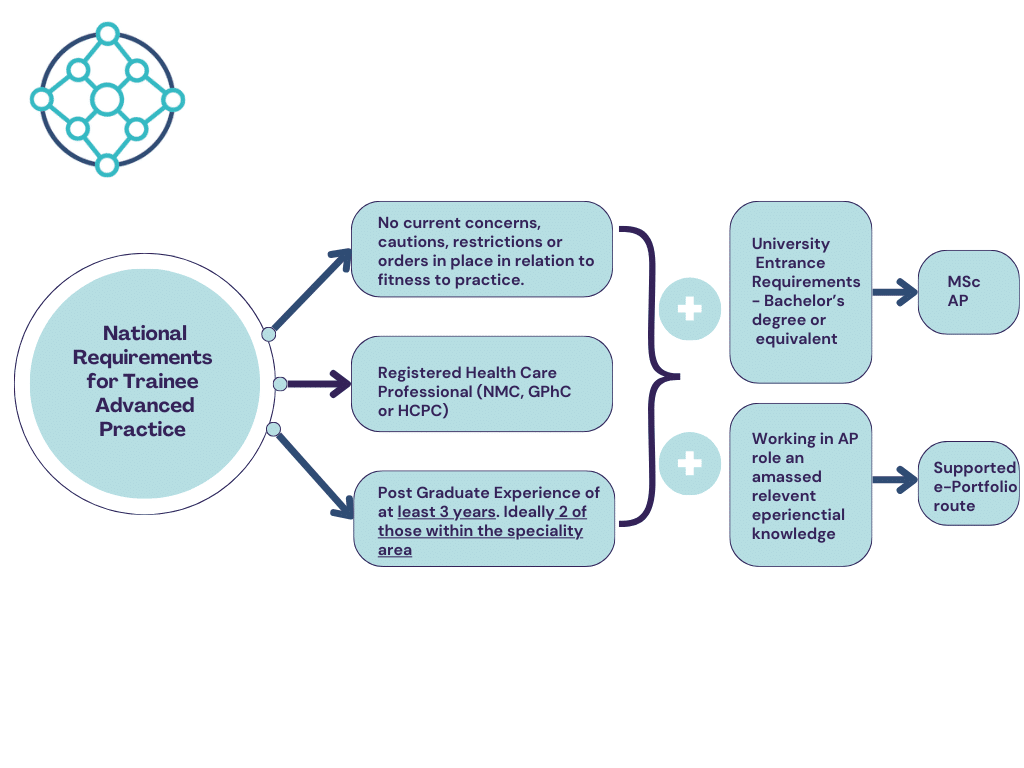
Who is/can become an Advanced Practitioner?
- Allied Health Professionals
- Nurses and Midwives
- Pharmacists
- Health Care Sciences
Physician Associates (PA):
PAs who are only working as GMC-regulated PAs cannot enrol on an AP course as they are not employed in a role with the autonomy of practice to undertake AP training. They would need to have both maintained their previous regulation as nurses/AHPs etc with another statutory regulator and have returned to a suitable autonomous role within that previous profession in order to be eligible for funding support for AP education & training.
Requirements:
- confirmation that the PAs have maintained their previous regulation as a nurse/AHP
- are/will be employed in a role as a nurse/AHP prior to commencement/application to the HEI for their Masters course as a trainee ACP.
ePortfolio (Supported) Route
The ePortfolio (Supported) Route provides formal recognition for experienced practitioners who:
- are currently working in advanced practice roles and have built up experiential knowledge equivalent to that of an MSc.
- completed their Masters before 2017 or through a non-accredited programme.
Although voluntary, completing this route demonstrates professional commitment and supports national recognition of advanced practice.
Why Choose This Route?
The ePortfolio (Supported) Route offers a structured, quality-assured process to:
- Showcase your existing skills, knowledge, and experience
- Evidence that you meet the Multi-professional Framework for Advanced Clinical Practice in England
- Gain formal recognition from the Centre for Advancing Practice
If you completed an accredited MSc after 2017, you may instead be eligible for recognition through an accredited programme.
How to Get Started
Review the eligibility criteria, obtain support from your employer or training provider, and submit an Expression of Interest (EOI).
Please note: Due to high demand, there may be a waiting period before you can begin. If you have already submitted an EOI, you do not need to submit another unless your details have changed.
MSc Advanced Practice
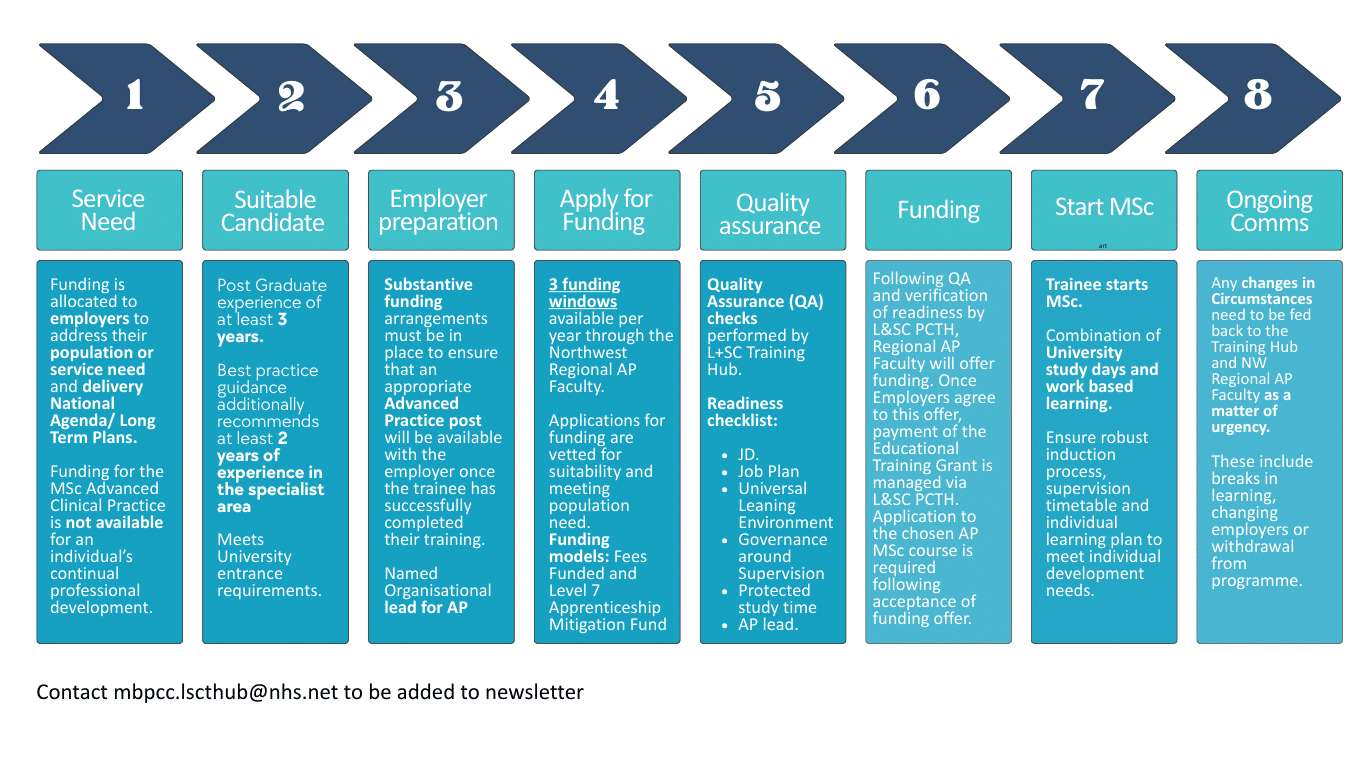
An employer should demonstrate population need by clearly showing local health demand, evidencing service gaps, providing data-driven justification, aligning with national priorities, and outlining the tangible impact an Advanced Practitioner will make on patient outcomes and system pressures.
Postgraduate Clinical Experience:
Candidates should have at least three years of post-graduate clinical experience, demonstrating a solid foundation in clinical practice, decision-making, and professional competence.
Specialist Area Experience:
Best practice guidance recommends a minimum of two years’ experience in the relevant specialty to ensure familiarity with the patient group, pathways, and clinical environment in which advanced skills will be developed.
Academic Entry Requirements:
Candidates must meet the university’s entry criteria, typically including:
- A relevant Level 6 qualification
- Evidence of recent Level 6 study
- Registration with the appropriate professional body
Fitness to Practise:
Candidates must have no current concerns, cautions, restrictions, or regulatory orders relating to their fitness to practise.
Check that you are ready to become a Trainee Advanced Practitioner by completing this checklist:
Substantive and sustainable funding arrangements must be confirmed to ensure that an appropriate Advanced Practice post will be available within the organisation once the trainee successfully completes their training. This includes securing long-term budget provision for the advanced-level role, demonstrating that the employer has a clear workforce plan, and ensuring the post aligns with service needs and strategic priorities. Employers should be able to show that the role will be permanently embedded within the team or service, with defined responsibilities, scope of practice, and salary line established.
The organisation must identify a Named Organisational Lead for Advanced Practice to provide oversight, governance, and strategic leadership for the development of Advanced Practice within the service. This individual is responsible for supporting the trainee, ensuring appropriate supervision and quality standards are met, and acting as the key point of contact with the Higher Education Institution (HEI) and NHS England. The Organisational Lead also helps to ensure alignment with local workforce priorities and maintains oversight of progression toward a substantive advanced practice role.
The North West Faculty for Advancing Practice offers support employer applications for MSc Advanced Practice training. These windows provide flexibility while ensuring fair and transparent allocation of funded places aligned to regional workforce needs.
Open Submission Window
Opens: November 2025
Closes: February 2026
The primary window for 2026/27 applications. Employers are strongly encouraged to apply during this period to maximise the likelihood of securing funding. Submissions must demonstrate service and population need, clear workforce planning, supervision capacity, and a substantive post to support the trainee on completion.
Late Submission Window
Opens: April 2026
Closes: June 2026
This window supports employers who could not apply earlier or whose workforce plans have changed. Applications are considered subject to remaining available places and continued alignment with regional and national priorities. All governance, supervision, and readiness requirements remain the same.
Waiting List Window
Open: September 2026
Closes: October 2026
This window allows employers to submit applications for candidates who meet all readiness requirements but could not be allocated a place during the main or late submission windows. Applications will be reviewed on a rolling basis and considered only if additional capacity becomes available. While placement is not guaranteed, submissions must still demonstrate full compliance with governance, supervision, and regional workforce priorities to be eligible for consideration
The Lancashire & South Cumbria Training Hub conducts comprehensive Quality Assurance (QA) checks to ensure that employers are fully prepared to host and support a trainee Advanced Practitioner. These checks help confirm that the learning environment, governance structures, and workforce plans meet the standards required for high-quality Advanced Practice training and that public funding is used effectively and responsibly.
The QA process includes a detailed review of the following Readiness Checklist components:
A clear, advanced-level job description must be in place, outlining the purpose, scope, and expectations of the trainee AP role. This ensures alignment with the four pillars of Advanced Practice and provides clarity for both the trainee and employer regarding responsibilities and progression.
Example of generic Job Description
A structured job plan must detail the trainee’s clinical duties, protected learning time, supervision arrangements, and developmental activities. This helps ensure balanced workload management and that the trainee can meet academic and practice-based requirements.
Example of generic Job Description
Example of Trainee ACP Job Plan
The employer must demonstrate that the placement area offers a supportive, inclusive, and high-quality learning environment. This includes access to multidisciplinary teams, opportunities to develop advanced-level competencies, and appropriate facilities to support education and reflection.
The ULE must be signed off by the Training Hub and General Practice Education Facilitators (GPEF) at least 3 months prior to trainees starting their Master’s Program.
Governance Around Supervision
Robust supervision structures must be in place, including identified clinical supervisors and appropriate governance frameworks. Employers must evidence processes for oversight, escalation, and assessment to ensure safe practice and compliance with national supervision standards. Further supervision guidance in the section below
Protected Study Time
Employers must guarantee protected study time to enable trainees to fulfil the demands of MSc-level learning and portfolio development. This typically includes a minimum allocation per week and must be ring-fenced within the job plan to support successful progression.
Advanced Practice Lead (AP Lead)
A named Advanced Practice Lead must be identified within the organisation to oversee the trainee’s progression, support governance, and act as the key point of contact for the Training Hub and HEI. This role ensures strategic oversight and consistency in Advanced Practice development.
Complete this self-assessment tool
Readiness-Checklist-for-Primary-Care-NHSE-NW-Faculty-for-Advancing-Practice-version-3.docx
What is funded
- There is also a special Mitigation Fund for Level 7 Apprenticeship routes: tuition + employer support are funded rather than through the apprenticeship levy.
- In addition, an Education & Training Grant is paid to the employer to support the learning environment (supervision, governance, study time, etc). This only applies to the fees funded on apprenticeship full MSc.
- Top-up modules are intended solely for learners who need up to three modules to complete the MSc in Advanced Clinical Practice within a twelve-month period. NHS England will fund tuition costs only, paid directly to the HEI. Learners requiring more than three modules to achieve the full MSc should instead apply for funding for a complete MSc programme. Those who already hold Level 7 credits—such as Non-Medical Prescribing (NMP)—should discuss Accredited Prior Learning (APL) with their chosen education provider, as this may shorten the duration of a full programme.
- Further funding guidance from NHSE
Education Grant: How much / payment mechanism
- A total of £30k is available for the full 3 year Masters Porgram
- The Training Grant is paid directly to the employer via invoice in arrears and based on enrolment and ongoing training. Money is received in instalments .
- Employers must ensure the trainee receives minimum 1 hour of supervision per week, and a minimum of £2,600 per year of the Education & Training Grant is stipulated to cover supervisory support.
- Once funding is approved, changes to start dates, education provider or funding route require prior approval; otherwise the employer may be liable for costs.
Once the trainee begins the MSc Advanced Clinical Practice programme, their development involves a structured combination of university-based study and work-based learning. Academic modules, simulation, and taught content are complemented by supervised clinical practice, allowing the trainee to apply advanced knowledge and skills within their workplace.
A robust induction process must be in place to ensure the trainee understands the expectations of the programme, their role within the service, and the support available to them. This includes orientation to clinical pathways, key policies, governance frameworks, and the advanced practice competency requirements.
A clearly defined supervision timetable is essential, outlining regular protected time for clinical supervision, educational support, and professional reflection. Supervisors should be appropriately trained and able to provide consistent guidance aligned to the four pillars of advanced practice – Advanced Practice Supervisor Capabilities – Advanced Practice
An Individual Learning Plan (ILP) should be developed collaboratively between the trainee, supervisor, and employer. The ILP identifies the trainee’s starting competence level, maps learning needs to practice opportunities, and sets out milestones to ensure progression throughout the programme.
Together, these elements ensure the trainee is supported, appropriately challenged, and able to develop safely and effectively into an autonomous Advanced Practitioner.
Any changes in circumstances must be reported to the Training Hub and the North West Regional Advanced Practice Faculty as soon as possible via the Change in Circumstance Form . Timely notification ensures appropriate support, accurate record-keeping, and correct management of funding and supervision.
Changes that must be reported include:
- Breaks in learning – e.g., sickness, maternity/paternity leave, or any planned or unplanned interruption.
- Change of employer – including moves within or outside the system, or changes to employment status affecting supervision or governance.
Any changes in circumstances must be reported to the Training Hub and the North West Regional Advanced Practice Faculty as soon as possible via the Change in Circumstance Form . Timely notification ensures appropriate support, accurate record-keeping, and correct management of funding and supervision.
Changes that must be reported include:
- Breaks in learning – e.g., sickness, maternity/paternity leave, or any planned or unplanned interruption.
- Change of employer – including moves within or outside the system, or changes to employment status affecting supervision or governance.
- Withdrawal from the programme – whether voluntary or advised by the HEI or employer.
Prompt reporting enables the Faculty and Training Hub to review implications, liaise with the HEI, and maintain safe and compliant programme delivery.
Withdrawal from the programme – whether voluntary or advised by the HEI or employer.
Prompt reporting enables the Faculty and Training Hub to review implications, liaise with the HEI, and maintain safe and compliant programme delivery.
Supervision
Supervision is an essential element of training to be an advanced practitioner. If you have been asked to supervise a trainee advanced practitioner, it is important to ensure you have the experience, knowledge, and expertise to provide good quality supervision.
Who can supervise
The Northwest Wider Workforce Clinical Supervisors course is a free RCGP accredited 2-day virtually delivered course for GPs and Advanced Practitioners who are currently supervising or plan to supervise the wider workforce in the near future. |
Minimum Standards
- Supervision for the trainee advanced practitioner is mandatory.
- The trainee must have a named, allocated co-ordinating education supervisor before commencing training in advanced practice.
- Throughout the period of training, there must be a minimum of one hour of scheduled supervision every week; of which one in four (once a month) is a scheduled hour with the co-ordinating education supervisor
- In certain practice contexts, where there is high risk, it will be necessary to debrief/provide daily supervision to ensure patient and practitioner safety.
Where a health professional is developing in advanced practice in a specialty/role with a nationally agreed curriculum, supervision arrangements should be guided by the relevant specialty curriculum.
Where no national curriculum exists, agreement of capabilities to be achieved at advanced level must be approved by the employer.
Supervision – Advanced Practice
Supervisor-readiness-checklist.docx
Advanced Practice Supervisor Capabilities – Advanced Practice
Employers-advanced-practice-supervision-action-plan.docx
Workplace Supervision for Advanced Practice
NHS England — South East » eLearning Resource for Advanced Practice Supervisors
Advanced Practice Supervision – a Multi-professional Learning Resource
RCN credential
From 27th June 2025, the RCN stopped credentialing of advanced nursing practice and are no longer accepting new applications or offer invitations to renew a credential to anyone listed on the RCN ALNP directory.
Does this affect you if you have completed credentialling already?
No. You will remain on the RCN ALNP directory which will remain open until 1st November 2028. You will remain on this until your 3 years lapses.
Does it make a difference if you are ARRS funded or not?
For AHPs working in Primary Care employed under the ARRS roles, the requirement is that they need to have a MSc (in AP) for their role to be reimbursed under ARRS, but they do not require a Digital Badge, so there is not an absolute requirement for these practitioners to have gained a Digital Badge* in addition to having completed an MSc.
Any AP nurses employed under the ARRS roles need a NHSE Digital Badge for new employment. This does not include existing or Non-ARRS funded roles.
For any AHPs/nurses/Pharmacists employed within primary care, where the ARRS scheme has not been used to fund their role, then it is up to their Employers to determine whether they have the capabilities to practice as an AP. Best practice guidance from CQC states that there would be an expectation that they hold an MSc (in AP) (or equivalent).
Useful resources
Refreshed Multi Professional Framework for Advanced Practice
2025/26 guide to implementing and funding Advanced Practice
Advanced Clinical Practice Nurses Primary Care England | Skills for Health
MSK Advanced Practice Framework
What's happening
ACP News & Events
CPD Training
Upcoming CPD training sessions, such as; Core People Management/Managing Culture, Collecting data, Prescribing safety, Project Management, Legal issues and more.
ACP Forum
Join the ACP Forum, hosted monthly on MS Teams.
Each month has a new topic and speaker.
Update - Credential
The RCN credential is not transferable / or currently recognised by HEE and Nurses have a choice to re-credential via the RCN or the Portfolio (supported) route. Therefore, anyone with an interest in moving to the HEE Portfolio route is encouraged to apply.
Launch of Governance Matrix
The link to the matrix (as well as a recording of the webinar) is available here.
If you have any questions regarding the implementation of the matrix into your organisation, please contact the Faculty via [email protected]
On 13th July, the Centre held a webinar to share the ACP Governance matrix which has been developed by a team led by James Pratt. This is a self-review document to assess where organisations have sufficient support and structures in place and where improvements are identified.
This is an important development across all areas of Advancing Practice and will be utilised by the Faculty to work with employers to create a safe and supportive environment for patients and ACP practitioners.
It provides opportunity for patients to receive timely care and negate unnecessarily delay in receiving treatment, especially with the growing shortage of GPs in primary care.
Lead new practice and service redesign solutions in response to feedback, evaluation and need, working across boundaries and broadening sphere of influence.
Continually develop practice in response to changing population health need, engaging in horizon scanning for future developments (e.g., impacts of genomics, new treatments and changing social challenges).
ACP within primary care enhances the effectiveness service delivery by enabling the practice to offer the right care, to the right patient at the right time.
ACPs in the primary care can develop close, long-term relationships with their patients and work in partnership with them to achieve optimum health.
Consider in your practice how training your own ACP could:
- Improve access to care delivery.
- Offer a sustainable solution to some of your succession planning.
- Consider what outcomes you would like to achieve for your practice. For more information or support, email [email protected].
Benefits to your practice could include:
- Embed a culture of learning and development
- Improve retention and resilience
- Enhance the skill mix within the practice
- Enhance the multi-professional team and help to provide safe, accessible and high-quality care for patients
- Form part of a sustainable business model
USEFUL MATERIALS
Resources & Videos
New resource alert!
Welcome to the new home of Teaching and Learning Consultation Skills (TALC Skills) and Healthy English: www.consultationskills.com.
TALC Skills covers all aspects of consulting with a patient, whether you are a GP or another healthcare professional, and aims to make consultations more enjoyable and more efficient.
These valuable free resources can be used independently by anyone who wants to learn or improve their consultation skills – or by educators. TALC Skills is an RCGP award-winner and its popular podcast has already received more than 28,000 downloads.
Healthy English has been developed to help everyone who works with patients become a better user of English. It addresses the language and communication needs of international health and care staff, their trainers and colleagues working in the UK.
Access to both of these resources is free of charge to NHS people and organisations.
Sign up and join hundreds of other colleagues across the country who are using this trending new resource.
Please find all recorded YouTube links below which are available to watch.
The Asthma and Pneumonia toolkits reflect the priorities in respiratory care including identification of risk factors, prevention, detection and diagnosis, medicines optimisation and reducing inappropriate secondary care admissions. They will support Respiratory Clinical Networks and clinical services to understand their priorities to improve patient care and outcomes.
The tool was developed by a group including representation from diabetes professionals and GPs around England and Wales. Feedback was obtained from diabetes professionals, GPs/APNPs, and the Primary Care Diabetes Society before producing the final version.
Links:
ACP
Meet Our Team

Phil Driver
Lead
